The International Classification of Functioning, Disability, and Health (ICF): A Global Model to Guide Clinical Thinking and Practice in Childhood Disability
Keeping Current © Debra Stewart, Peter Rosenbaum, 2003
Introduction: Why is This Topic Important?
The International Classification of Functioning, Disability and Health (ICF) (WHO, 2001) is a classification system developed by the World Health Organization that focuses on the 'components of health'. It encompasses all aspects of health and describes them in terms of health domains and health-related domains. It is intended to be a universal classification system, meaning that it is about all people, not just people with disabilities.
The primary purpose of the ICF is as a classification system, i.e., to code the components of health. It is intended as a complementary classification system to the WHO's International Classification of Diseases (ICD). The ICF manual also includes a new model of human functioning and disability (Figure 1) to reflect current views of the interactive relationship between health conditions and contextual factors. This purpose of this Keeping Current is to describe and discuss the ICF model as a useful tool to guide clinical thinking, practice, education and research in the field of childhood disability.
Figure 1: The ICF model
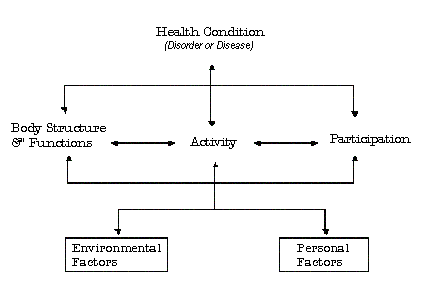
Historical background
In 1980 the World Health Organization (WHO) published the International Classification of Impairments, Disabilities and Handicaps (ICIDH) (WHO, 1980). The ICIDH was a classification of the "consequences of disease", developed by the WHO as part of a family of classifications to code a wide range of information about various aspects of health. The original ICIDH included a conceptual model in which 'diseases' and 'disorders' were linked to their possible consequences, specifically 'impairments', 'disabilities' and 'handicaps' (Figure 2). The model helped people see that a consideration of 'disease' alone provided an incomplete perspective of health status. It also encouraged people to recognize the impact of a disorder on an individual's function and capacity to engage fully in their lives.
Figure 2: The original ICIDH model (WHO, 1980)
disease —> impairment —> disability —> handicap
Many countries did not use the classification system, and the original ICIDH model was viewed by many people as problematic. Among the concerns expressed by some people who used the ICIDH, including people with chronic health conditions, was the negative portrayal of the consequences of diseases in terms of 'disability' and 'handicap'. People were also concerned about the linear (and unidirectional) connections among the elements of the ICIDH model. This biomedical approach to disease has utility in many areas of health care (e.g., in diagnosing the bacterial agent in many infectious diseases, leading to treatment with appropriate antibiotics). On the other hand, taken alone, it presents a rather narrow and limiting way of considering chronic health conditions in childhood such as cerebral palsy and developmental disabilities, where specific 'causes' are often unclear.
In the early 1990s an international effort was begun to revise and reshape the ICIDH. After nine years of study and input, the WHO published the new classification system: the International Classification of Functioning, Disease and Health, or ICF (WHO, 2001). A new model of human functioning and disability (Figure 1) was also presented.
A model of human functioning and disability
The World Health Organization's two models of health and disability that were published in 1980 and 2001 respectively demonstrate how global views about health and disability have changed in a relatively short time. One key change is a shift in language from negative terms such as 'impairment', 'disability' and 'handicap' to the neutral terms 'body function and structure', 'activity', and 'participation', respectively. The appendix at the back of this report provides definitions and examples for the key terms of the ICF.
A second change is that the term 'disability' is now an umbrella term to represent the dynamic interaction between person and environment. In contrast to the traditional view that disability resided just within the person this change reflects the idea that 'disability' is a social construction involving an interaction of the person and their community or society. As well, the change in terminology reflects a move toward the identification of 'participation' as an important dimension of health. A significant modification in the model was made when the implied linear connection between 'impairment', 'disability' and 'handicap' was changed with the inclusion of a series of bi-directional arrows that link these (and other) elements of health, functioning and disability. Because all the components of the model are now linked to each other, the possibility that any aspect of function can and probably will affect another, in a non-linear manner, is formally recognized. Thus, for example, it is possible to explore the impact of a change in an individual's 'participation' on their 'activity' and even the expression of the 'impairment' that may underlie the functional challenges. This systemic way of thinking is more dynamic than the linear connections presented by the original ICIDH model.
Two significant additions to the original ICIDH model reflect recent views about the social construction of health and disability. They are classified as contextual factors that may impact a person's health state. The first contextual component is 'environmental factors' which can be physical, social, cultural or institutional in nature. The second component is 'personal factors' such as gender, age, education and lifestyle. These two contextual factors influence and modify other components of disease or disorder, and need to be identified and considered in the mix of forces that together contribute to the dimensions of 'body function/structure', 'activity' and 'participation'.
To summarize, the WHO chose a 'biopsychosocial' approach to health, functioning and disability in the new ICF model, in order to provide "a coherent view of different perspectives of health from a biological, individual and social perspective" (WHO, 2001, p. 28).
Use of the ICF: Why is it important?
The World Health Organization is encouraging application of the ICF internationally not only as a classification tool, but also as a framework for social policy, research, education and clinical practice.
It is our impression that unlike its ICIDH predecessor, the ICF model of human functioning and disability appears to have captured people's attention very quickly following its publication. This may reflect the change in emphasis from disease to health, or perhaps the incorporation of 'environment factors' and 'personal factors' that round out what might previously have been seen as a view of the world that was too narrow and 'medical'. Whatever the reasons, we believe that the ICF needs to be disseminated widely and understood by all people working in health care, research, and education, as it offers a global framework of health and health-related states. It provides a common language for describing health, functioning and disability, which will be used worldwide.
Service providers in Canada may not wish, or need, to use the ICF as a classification system, however, the model of functioning, disability and health described in the ICF "provides the building blocks " (WHO, 2001, p. 25) for clinical and research applications. Although it is recognized that no model is perfect, the ICF model does represent current world views of health and disability, and it is already being used in many countries for multiple purposes..
In the rest of this 'Keeping Current' we will outline some thoughts about the ways that the ICF model can be used to guide clinical thinking and the delivery of services in the context of childhood disability.
The ICF and 'Clinical Thinking'
In the field of childhood disability, the ICF model of functioning and disability provides many more 'points of entry' for people seeking both to enhance activity and participation of children whose functional well-being is at risk, and to prevent secondary impairments. The first and most obvious factor to identify is that the 'environment' around a child involves their family. In an 'ecological' way of thinking the family is the context in which children develop. When the family 'environment' is recognized as contributing to children's ultimate well-being, efforts to support families (such as implementing and practicing family-centred service [FCS]) are important corollaries of this thinking. Furthermore, in addition to the philosophical principles of FCS (Rosenbaum et al., 1998), and the established connection between FCS and overall parent satisfaction and mental health (King et al., 1999), it has been shown that families can participate in the identification of goals for their children's therapies. In so doing they can help their children achieve greater functional gains, with less effort, than are seen with traditional impairment-based therapy (Ketelaar et al. 2001).
Another issue that emerges from this expanded way of thinking about functional well-being involves recognizing the differences between people's 'capacity' and 'performance' (Tieman, 2002; WHO, 2001). These are two terms that the WHO has introduced as qualifiers to the Activities and Participation component of the new ICF. The 'capacity' qualifier describes an individual's ability to execute a task or action at the highest probable level of functioning. The 'performance' qualifier describes what an individual actually does in his or her current environment (WHO, 2001). Table 1 below outlines an information matrix proposed by the WHO to differentiate these concepts. Although these new qualifiers have not been tested yet, they do provide us with a way of thinking about health and disability at individual and societal levels of functioning.
Table 1: Activities and Participation Information Matrix (WHO, 2001)
Domains
Performance
- Learning and applying knowledge
- General tasks and demands
- Communication
- Mobility
- Self-care
- Domestic Life
- Interpersonal interactions and relationships
- Major Life Areas
- Community, social and civic life
Qualifiers
Capacity
Service providers assessing children with disabilities usually want to know what the child is capable of doing at their best (their 'capacity'). For example, to evaluate the mobility capacity of a child with cerebral palsy, we will usually do our assessment in an environment most conducive to the child's best performance. We will use a barrier-free environment, with smooth surfaces and as few obstructions as possible, often in a laboratory or clinic setting. Of course in natural environments (such as home, school and community) many surfaces are uneven, the hallways are crowded and there may be stairs to be negotiated. In this way, the school-based 'performance' of independent mobility may be quite different from the clinic-based 'capacity' of a child. Service providers must be aware of the possibility of these differences in the activity and participation levels of the children they see. The ICF model can help to guide people to acknowledge and accommodate differences in functioning at different levels. For example, when a person's participation in moving around the community (mobility) is restricted, service providers can address both capacity and performance, and identify factors that are influencing mobility. Often, environmental factors influence a child's ability to move around in the community, and thus mobility aids become a viable intervention to narrow the gap between a person's capacity and desired performance in the community. Note that the 'impairment' has not (in this example) been addressed at all, but the net benefit to the person may be considerable improvement in function. (It is also possible - even likely - that as mobility function is enhanced there may be changes (improvements) in underlying impairments such as muscle strength, body alignment, weight shift or stability.)
How do 'personal factors' enter into the discussion? Traditional thinking has often involved a belief that children with disabilities should be encouraged to try as much as possible to learn and to do things 'normally'. Interventions have taken 'normal' as the guidepost by which to structure what we prescribed and recommended. This approach does not factor in or take advantage of the preferences for activities that a developing child might want to do, or to avoid. The formal acknowledgment of the 'personal factors' component of the ICF model recognizes the importance of personal choices, interests, likes and dislikes of the person whose 'activity' and 'participation' are being addressed in a therapy program. In fact it is likely that the impact of the 'functional therapy' approach reported by Ketelaar et al. (2001) had much to do with the self-chosen goals pursued by the children and parents in the experimental group. People are simply more likely to work at things that are important to them than at things others feel are important, even if they really are important!
The ICF model 'gives permission' to address people's self-determined goals very broadly. These might, for example, include becoming 'independently mobile' or being able to 'communicate effectively', rather than focusing only on 'walking' or 'talking'. This emphasis argues that what people do is more important than that they do things 'normally'. In this sense the model asks us to accept variation and difference, to celebrate the achievement of self-defined goals accomplished in whatever ways are best for us with our particular and unique range of skills and limitations.
How Can I Use These Ideas in Practice?
(i) In the assessment stage of clinical practice, health care providers are encouraged to use the ICF model to guide the selection of their approaches to measuring the outcomes of interest to their interventions, and to link measured outcomes to goals and the decision-making processes that influenced the choice of those goals. Our outcomes need to be multi-dimensional, in order to encompass functioning at different levels of body function and structure, activity and participation. Equal emphasis should be placed on determining the influence of personal and environmental elements on a person's overall health and well-being. New outcome measures are being developed that provide us with the tools we need to evaluate the effectiveness of our interventions at the participation level (Coster, 1998; Law et al., 1998; Missiuna & Pollock, 2000). Taking this wider view will also enable us to explore the interconnections across measures of the different dimensions of people's health and functioning.
(ii) In intervention, many clinicians provide counseling and education to families of children with developmental disabilities. One of the tasks of service providers is to relate how our therapeutic activities are connected to the desired outcomes. An impairment-based approach to treatment addresses primarily the problems of body structure and function thought to underlie the functional limitations of the 'disability. There is at least an implicit assumption that 'treatment' will produce functional results, and perhaps an unspoken belief that more therapy will produce better results.
The ICF model provides an opportunity - from the outset - to talk with parents (and older children) about a different set of primary goals - goals that address function ('activity') and social engagement ('participation'). In this way of thinking impairment-based interventions may still play an important role in management; but now the focus widens, so that additional perspectives gain currency and can be considered equally valid ways of encouraging children to become functional. For example, a child with a disability that affects oral motor control may benefit from assessment and intervention focused on the motor impairment, but service providers who also address the activity of eating and the child's participation in family mealtimes, as well as alternative communication strategies, as necessary, are ensuring that all components of the child's functioning and health are addressed.
These comments are in no way meant to diminish the role or importance of 'impairment-based' interventions, but simply to recognize that interventions at any (perhaps all) of the components of the ICF model may be important, appropriate, and interlinked. Bartlett and Palisano (2000, 2002) have presented thoughtful ideas about the ways to incorporate the ICIDH/ICF models into aspects of clinical decision making in physiotherapy, in part to recognize opportunities for prevention of secondary impairments often associated with developmental (and of course other) conditions.
(iii) In the ICF model, the environment in which the person with a disability lives is important and needs to be considered in the course of planning and delivering interventions. This orientation is consistent with models that consider 'person' and 'environment' as dynamic and interactive dimensions of an individual's situation, such as Bronfenbrenner's 'ecological' model (Bronfenbrenner, 1977) and the Person, Environment, Occupation (PEO) model in occupational therapy (Law et al., 1996).The ICF model acknowledges that the contexts in which people live their lives play a central role in the expression of their capacity to function. In the context of childhood disability this may mean allowing, even encouraging, the liberal use of 'augmentative' interventions such as mobility aids, alternative communication devices and related technical tools, which can have an important role in the lives of people whose functional abilities can be enhanced with such interventions. Furthermore, the social and cultural environment must be considered in assessment and intervention, as we know that other people's attitudes, values and beliefs affect a child's participation in daily activities (Law et al., 1999).
(iv) Managers and decision makers in the field of childhood disability can use the ICF model and classification system to guide the development of policies and procedures that reflect current views and beliefs about the biopsychosocial nature of health and disability. In Ontario, for example, the Professional Advisory Committee of the Ontario Association of Children's Rehabilitation Services (OACRS) has been working with the ICF model to design a Framework for Care Management Tools that can be widely applied.
(v) Researchers and educators are also encouraged to apply the ICF model to their practice. Studies on childhood disability should include dimensions of activity and participation, and environmental factors, to capture the complex, interactional nature of the life experiences of children with disabilities and their families. We also have a professional responsibility to study the application of this new model, and to provide critical feedback to the World Health Organization. Educators need to inform future health professionals about the ICF, as it represents a global framework and common language that will be used to describe and classify health and health-related states.
Summary
The World Health Organization is encouraging people around the world to view health, disability and functioning as dynamic and interactive concepts that recognize person and environment factors as equally important. The new ICF encourages service providers, managers, researchers and educators to adopt a biopsychosocial approach to service delivery that addresses health and disability from biological, individual and societal perspectives.
Update written by:
Debra Stewart, BSc (OT), MSc, Co-Investigator, CanChild, Assistant Clinical Professor, School of Rehabilitation Science
Peter Rosenbaum, MD, FRCP(C), Professor of Pediatrics, McMaster University and University of Toronto, Co-Director of CanChild
Want to know more? Contact:
Debra Stewart
CanChild Centre for Childhood Disability Research
Institute for Applied Health Sciences, Room 408
1400 Main St. W., Hamilton, ON L8S 1C7
Tel: 905-525-9140 x 27850 Fax: 905-522-6095
canchild@mcmaster.ca
